The Missing Kingdom: Why Fungi Must Be Central to Conservation Strategy
28 December 2025
Published online 5 March 2013
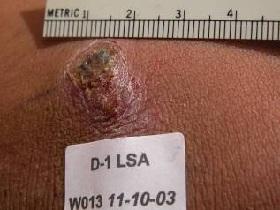
Cutaneous leishmaniasis can be caused by several different species of the Leishmania parasite, including Leishmania major. In recent years, these parasites have grown resistant to antimony-based drugs, the standard therapeutic approach, and there are no safe and easy-to-use alternatives.
Now, an international research team has demonstrated a promising topical treatment using the antibiotic creams paromomycin and gentamicin1.
The team, including researchers from the US Army Medical Materiel Development Activity, the Institut Pasteur in Tunis and Paris, and the Tunisian Ministry of Health, conducted the study in Tunisia with 375 patients with cutaneous leishmaniasis. The patients were divided into three groups, which received a mixture of paromomycin with gentamicin; paromomycin only; or a control treatment. The patients, aged between 5 and 65, were given the topical cream once daily for 20 days.
On its own, paromomycin healed the ulcers caused by cutaneous leishmaniasis with an efficacy of 82%. A similar result was found when it was combined with gentamicin (81%). The results contrasted significantly with the control group, in which ulcer healing was only observed in 58% of the patients.
Although the addition of gentamicin did not seem to improve efficacy, in previous studies on mice it did increase the rate of cure when combined with paromomycin in some cases.
A typical patient response to treatment was a reduction in ulcer size by 42 days, with complete healing by 98 days. Few ulcers relapsed by the end of the trial (168 days), and the researchers reported an acceptable side-effect profile, with no patient withdrawing from the study owing to adverse events.
"This treatment has the potential to become a first-line treatment for uncomplicated cutaneous leishmaniasis patients," says Max Grogl, a co-author of the study.
doi:10.1038/nmiddleeast.2013.29
Stay connected: