The Missing Kingdom: Why Fungi Must Be Central to Conservation Strategy
28 December 2025
Published online 1 December 2013
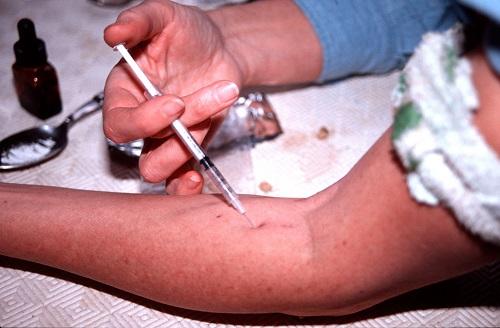
Efforts in the Arab world to reduce HIV transmitted through drug use and prostitution are undermined by a moral objection to these activities and the fear that making them safer could be seen as condoning such behaviour.
Should health workers provide intravenous drug users with free needles, and give sex workers condoms to reduce the risk of HIV transmission? In the Middle East and North Africa (MENA) — one of only two regions in which HIV rates continue to rise1 — such suggestions are met with varying degrees of resistance.
In the MENA region, only Lebanon, Morocco, Jordan, Tunisia and Syria explicitly support a harm minimization approach as part of official strategies to reduce HIV transmission through drug use2. There is widespread concern that such initiatives, by making the behaviour in some way safer, tacitly condones or encourages illegal activity.
"There is a misunderstanding that reducing harm implies accepting a behaviour or even encouraging it," says Alex Smolak, a research consultant at the Infectious Disease Epidemiology Group at Weill Cornell Medical College in Qatar and a research affiliate at the Global Health Research Center of Central Asia at Columbia University.
While people may readily accept harm reduction measures in the food or beverage industries — where cigarettes are filtered or lower-calorie drinks produced — similar efforts are a long way from being accepted in the context of HIV, says Smolak. "The stigma related to HIV risk behaviour prevents some people from being able to focus on the public health issue."
Needle and syringe exchange programmes (NSP) exist in the region, but without any nationwide strategies. They are largely funded by international organizations and implemented by NGOs who work with high-risk groups including people who inject drugs (PWID), female sex workers, and homosexual men.
In the case of Egypt, there is a limited service focusing primarily on PWID, offering free distribution of needles and condoms3. HIV prevalence in Egypt is quite low (below 0.02% of the general population), but it rose sharply among PWID from 0.6% in 2006 to 6.7% in 20104.
Doaa Oraby, an independent consultant with extensive research experience on HIV in Egypt, says this significant jump justifies targeting PWID for harm reduction in Egypt. "Once you pass [the] 5% [margin of infection] among a particular group, the potential for rapidly escalating transmission rates becomes significant," she says.
In Oman, though no formal harm reduction programmes distribute sterile injecting equipment, there is anecdotal evidence of small-scale, unofficial syringe distribution in areas around Muscat2.
In Bahrain, sterile injecting equipment requires a medical prescription for purchase. Reports of arrests on the basis of possessing drug paraphernalia such as new needles and syringes are common5. With no harm reduction strategy, 58% of transmission of HIV in the small island is attributed to intravenous drug use2. The shortage in the supply of new needles and syringes is reflected by the country's high rate of syringe-sharing, at 53.4% according to one survey5, one of the region's highest.
Alongside needle and syringe programmes, opioid substitution therapy (OST) is another method of harm reduction targeting PWID. This approach aims to replace illegal opioid drugs such as heroin with a slow release and less euphoric alternative, usually methadone, taken orally under medical supervision.
Only Morocco and Lebanon approved alternatives such as methadone and buprenorphine as part of OST, and achieved positive results2. The Omani government approved an OST pilot programme last year, but never launched it.
OST is a controversial approach to harm reduction, more so than NSP, even among some public health experts. "It's not yet clear if its benefits outweigh it harms, at least in Egypt," says Oraby. Methadone is not easily available in Egypt, and some, like Oraby, are concerned that Egypt's lax regulations may only exacerbate drug abuse if it is made available.
Political instability in the region has affected all development programmes in general
Harm reduction approaches in the region suffer due to a lack of surveillance and resultant knowledge of where efforts will have the most impact, Smolak says.
While PWID are at the centre of harm reduction strategies relating to HIV, there is limited and often unreliable data about this group and its behaviours. For instance, estimates of the number of PWID in the Middle East and North Africa, including Israel and Iran, can vary from 300,000 (ref.6) to one million (ref.7).
Despite an increase in the number of countries that conduct bio-behavioural surveillance of HIV high-risk populations, data on HIV testing, prevalence, and antiretroviral therapy (ART) are still largely sourced from police registers, detoxification services, and prison records2. The available numbers could be subject to reporting bias.
There is also a lack of data on what proportion of ART recipients are PWID2. For instance, in Libya there were around 2,500 HIV-infected people receiving free ART in 2012. But there is no data available as to how many of them are PWID, although in the past, injecting drug use was known to have been the cause for as much as 90% of HIV transmissions in Libya8.
HIV-related harm reduction can meet even greater resistance when the state is asked to fund the reduction of harm for stigmatized activities among convicts.
Iran is the only country in the region that provides NSP or OST for incarcerated drug users, despite evidence of injecting equipment being habitually shared in prisons across Lebanon, Kuwait, and Jordan2. And yet, limited data from MENA suggest that significant numbers of PWID spend time in prison, often continuing to inject drugs and sharing needles while incarcerated – examples include Syria9 and Oman2.
Another concern is evidence of non-drug users becoming PWID while in prison. For instance, a 2011 survey of inmates in Lebanon's Roumieh prison found that 34% began using drugs while incarcerated, with 37% of them injecting10.
Morocco is the only country in the region to provide HIV awareness programmes for prisoners and prison managers and the country plans to introduce OST in its prisons in the future2. In Libya, a US$6m HIV awareness project focusing on PWID in prisons was relaunched by the government last year. Outreach programmes include HIV testing in prisons, including training and awareness among inmates and staff.
The general consensus in the region is that while the need for harm reduction is recognized, it requires more domestic public and financial backing. Currently, the majority of MENA countries rely on external funds for at least 50% of their harm reduction responses2.
"It's also true that the political instability in the region has affected all development programmes in general," says Oraby.
Smolak adds that while public health would benefit from increased harm reduction programmes for PWID, initiatives should also target female sex workers and men who have sex with men — the two other higher-risk groups for HIV. These groups are possibly more stigmatized in the region than PWID and receive minimal funding for harm reduction strategies, except for some government and NGO programmes in Lebanon, Tunisia, Algeria, and Morocco that provide them with condoms.
Efforts to destigmatize different groups will possibly be incorporated within future harm reduction strategies. A recent Egyptian film, Asmaa, which gracefully recounts the true story of a woman struggling with HIV, is cited by Harm Reduction International as an example to be emulated.
"The next step for harm reduction in the region could be pairing stigma reduction programmes with harm reduction programmes," says Smolak.
doi:10.1038/nmiddleeast.2013.231
Stay connected: