Understanding longevity: From gene sequences to social inequity
03 April 2025
Published online 1 December 2013
Policies that accommodate sociocultural factors must be adopted in the Middle East, a region still with a strong opportunity for prevention.

The adoption of evidence-based HIV policies could help prevent the spread of HIV in the Middle East and North Africa (MENA), a region whose low HIV prevalence puts it within the realms of possible recovery from the epidemic.
But weaving HIV prevention policies into the sociocultural fabric of MENA countries is fraught. Much international HIV policy research is carried out within a Western liberal framework; based on varying degrees of tolerance towards the behavior of at-risk populations, such as homosexuals or sex workers.
There is evidence that the HIV epidemic in MENA is concentrated among three key populations: people who inject drugs (PWID), female sex workers (FSW), and men who have sex with men (MSM). Unless HIV is controlled in these key populations, it will continue to move into the general population — after all, they are interconnected.
For example, a husband who has sex with a FSW and becomes infected could pass the virus to his wife. Similarly, studies have found that many PWID and MSM in the region are married.
But some commentators in MENA countries argue that Western-style HIV policies advocate a worldview that conflicts with the region's conservative values. Some go further and say these international policies are a form of neocolonialism or cultural imperialism.
The situation begs the question: How can the region reconcile HIV preventive polices and its sociocultural norms?
One solution lies in making a clear-cut distinction between endorsing culturally unacceptable behavior and addressing a concern for public health. Iran and Malaysia are not Arab nations; however having a Muslim majority, they share some similarities with MENA countries. Islamic scholars in both of these nations have lent their support to harm reduction measures aimed at key populations in order to benefit public health.
From there, NGOs have become a conduit for directing funding to harm reduction efforts. In both Iran and Malaysia, needle exchange services are available to PWID, and are showing good results in reducing HIV transmission.
A partnership between researchers, Islamic scholars, policymakers, advocates, and NGOs is essential for policy change in MENA. Current data could be presented to Islamic scholars in order to gain their support. This support will lessen stigma, thus helping policymakers, and in turn NGOs which implement harm reduction policies.
Successful policies in MENA have led to most countries in the region providing antiretroviral treatment (ART) free of charge to people living with HIV (PLHIV). However, UNAIDS estimates that only 10% of PLHIV in need of treatment in MENA are receiving it – among the lowest coverage in the world.
The treatment of HIV with ART has been shown to reduce viral counts to undetectable levels thereby reducing the likelihood of transmission.
The low ART uptake is multifactorial, but a major reason could be that many people do not know their HIV status. Readily available testing and less stigma will encourage people to learn their HIV status. In addition to addressing these broader issues, incentives to encourage sticking to an ART programme can improve effectiveness. Financial incentives in the form of small payments for taking ART, proven by blood tests, have been found to increase adherence.
It is difficult for many healthcare professionals to offer HIV testing to patients for fear of causing offence at the suggestion that the patient has engaged in taboo behavior. The region therefore needs to create policies that encourage, or even obligate, healthcare providers to offer HIV screenings. Mandatory testing may help lift the stigma.
The picture is not all bleak. There are several examples of successful evidence-based policy and NGO activities in the region. Tunisia has an effective health screening programmes for FSW. Egypt and Algeria both have HIV testing and education programmes for FSW. Morocco has initiatives to address HIV prevention among FSW and MSM. Tunisia and Algeria have put forward outreach programmes to MSM to encourage condom use and HIV testing. Jordan has advertisements on buses directing PWID to treatment resources. Egypt has several NGOs that provide clean needles to PWID. Lebanon has developed prevention programs for all three key populations.
These programmes are all encouraging, but efforts are hindered by lack of funding and overcautious state support, which often takes the form of governments publicly disassociating from programmes.
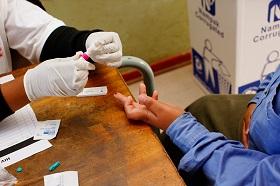
© Hoberman Collection / Alamy
Several countries in the region are home to a significant number of migrant workers, who are HIV vulnerable, according to many studies. Usually, workers testing positive for HIV are immediately deported. However, deportation does not address the fact that many migrant workers often get infected with HIV while in the host country.
For instance, separation from spouses coupled with greater access to financial resources can contribute to risky behavior, such as having intercourse with sex workers. HIV prevention focused on key populations will address the transmission source in the host country and reduce fresh HIV contraction among migrants.
But first, HIV prevention efforts — including education, awareness and free voluntary testing and treatment — must be made easily accessible to migrant workers.
As such, it is valuable for policies to acknowledge the contextual and structural factors for many HIV-risk behaviors; an integral part of HIV prevention policy.
Another important policy issue lies in the empowerment of women, to increase their ability to refuse sex that may put them at risk for HIV. Research has found that more educated and financially secure women are less likely to engage in transactional sex or sex with someone who is known to engage in high-risk behaviour1,2,3.
The region continues to make strides in this area – such as improving women's access to education – but it can strive to improve further. Education is also vital for two other vulnerable populations; youth and prisoners.
And policies that facilitate homegrown research on HIV and international collaboration must be encouraged. But for epidemiological and intervention research to reach its full potential, the key is to understand the region's culture. Insight into the way society works can provide much strength in the fight against HIV, and recognizing this is essential for recreating and aligning policies in a way that can enhance HIV management efforts.
Alex Smolak is a research consultant at the Infectious Disease Epidemiology Group at Weill Cornell Medical College in Qatar and a research affiliate at the Global Health Research Center of Central Asia at Columbia University in New York City. He holds a PhD from Columbia University and is a Fulbright alumnus.
doi:10.1038/nmiddleeast.2013.230
Stay connected: