The Missing Kingdom: Why Fungi Must Be Central to Conservation Strategy
28 December 2025
Published online 4 March 2011

Hepatitis C remains a neglected disease in Egypt despite it infecting an estimated 500,000 Egyptians each year. Central to combating this deadly disease is an efficient diagnostic tool capable of widespread population screening.
This technology is the goal of chemist Hassan Azzazy, associate dean of graduate studies & research at the American University in Cairo (AUC). He and doctoral student Sherif Shawky turned to the burgeoning science of nanotechnology to find ways to directly detect viral RNA in a blood sample.
Their first experiments involved adding minuscule specks of gold — or 'gold nanoparticles' — to a chemical mixture that contains short DNA strands with a complementary sequence to that of the virus.
This effectively allowed these nanoparticles to recognize viral RNA and congregate around it — like small pieces of iron clinging to a magnet.
The key lies in the unique properties of the gold nanoparticles. Normally, they exhibit a phenomenon called 'surface plasmon resonance', which gives the particles an intense red hue. Yet, when these nanoparticles gather close together, such as when they are drawn to the virus's RNA, they appear blue.
The primary colour red is itself somewhat problematic. "It's obviously the same colour as blood, so we won't be able to [distinguish] it," explains Azzazy. This makes it difficult to monitor the diffusion of the gold nanoparticles within a blood sample.
"Because of this, we have to use serum samples, [which can be easily extracted from blood samples] and administer the test to them instead because serum has a pale yellowish colour."
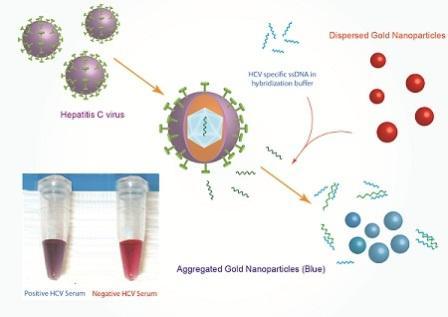
The chemical solution containing the nanoparticles can then be added to the serum sample. If the colour remains red, the virus is not present. If it shifts to blue, the sample is positive for HCV infection.
The diagnostic test for HCV in use today is a twofold process. Individuals are first tested for HCV antibodies. If there, the person was exposed to HCV, but the virus is not necessarily still active.
If positive, RT-PCR (PCR with reverse transcription) is performed, which amplifies any viral RNA present in a blood sample. In theory, HCV infection can be diagnosed with only the expensive RT-PCR, but owing to its higher cost, the cheaper antibody test is administered first.
"What we are trying to do is cut down on the time and cost of this entire diagnostic process," says Azzazy. On average, both tests cost approximately 70 USD. "It is a time consuming and expensive process that many Egyptian cannot afford to pay."
Azzazy claims that using gold nanoparticles to directly detect the virus's RNA will cost one tenth of the current diagnostic procedure, taking no longer than half an hour. He also notes that this procedure cuts the risk associated with relying on negative antibody tests.
"It's important to detect the virus directly because it is possible that you are still infected by HCV even if you don't find any antibodies associated with it in your body," Azzazy warns. For instance, it may be that the individual was too recently infected for the antibodies to appear. Also, a false negative result might occur owing to a weakened immune system or a variety of other rare circumstances associated with HCV or the body.

© University of Hawaii
Nevertheless, other researchers remain skeptical about how useful advances in the diagnosis of HCV will be in stopping the spread of the disease. DeWolfe Miller, an epidemiologist at the University of Hawaii, Honolulu, and one of the people who uncovered the endemic transmission of HCV in Egypt in the 1990s, is unconvinced.
"I know it sounds counter-intuitive, but improved screening techniques will not help at all in prevention," says Miller, who is currently in Cairo looking for funding to set up a prevention program in post-revolution Egypt.
For him, the key is to directly reduce exposure to the virus rather than better diagnostics.
"There are now relatively few cases of the virus being transmitted via blood transfusion in Egypt, thanks to a law that requires all donated blood to be screened for HCV," say Miller. While that screening process may not always be perfect, he admits, the vast majority of transmissions are now caused by medical examinations or treatments.
"It's through the injection you get at the dentist, the nurse's gloves that aren't changed often enough, the multi-dose vials that are used to inject dozens of people," says Miller.
Azzazy agrees that prevention is crucial, but insists that widespread testing is equally important. "The problem is that people don't know," he says. "How can you protect others if you don't know your HCV status? A person who's aware of [their] positive HCV status would not donate blood and would exercise proper measures to prevent spreading it to his family."
The use of gold nanopaticles to diagnose HCV is awaiting FDA approval, though the researchers have already filed for patents in the United States and internationally. A spin-off company is currently being established in Egypt to market the technology.
Azzazy is hopeful that the basic technique behind this application can be scaled-up to diagnose HCV infection and other diseases such as tuberculosis cheaper and faster.
Diagram Credit: "Novel Diagnostics and Therapeutics Research Group" in Yousef Jameel Science & Technology Research Center at AUC.
doi:10.1038/nmiddleeast.2011.27
Stay connected: