River subbasins more depleted than
official figures show
09 April 2024
Published online 17 August 2010
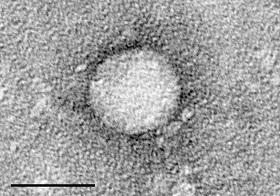
On average, over half a million people in Egypt get infected by the Hepatitis C virus (HCV) each year, far more than any other country in the world, according to a new study published in the Proceedings of the National Academy of Sciences.
The epidemic has raged in the country for several decades now and shows no signs of abating. Nearly seven out of every 1,000 of Egypt's 77 million people get infected each year. Around 10% of Egyptians are chronically infected and infectious, creating a large reservoir that supplies the spread of the disease, mainly through hospitals and clinics.
Laith Abu-Raddad, co-author of the study and assistant professor of public health at the Infectious Disease Epidemiology Group, Weill Cornell Medical College in Qatar, compared the Hepatitis C disease burden in Egypt in several respects to the HIV/AIDS epidemic in sub-Saharan Africa. "[We have] millions of cases of an infection for which there is no vaccine, no effective treatment, and where case management is so expensive that it is beyond the reach of most patients."
The researchers examined representative, peer-reviewed reports of HCV in Egypt published since 1992. Using this data, they applied epidemiologic models to estimate the rate of incidence. The staggering number of annual infections is much higher than previous estimates by the Egyptian Ministry of Health and Population.
Wahid Doss, head of the National Committee for the Control of Viral Hepatitis (NCCVH), challenged the results, calling the numbers exaggerated. He told Al-Masry Al-Youm, an Egyptian daily newspaper, that according to the NCCVH latest surveys, the number of new infections each year lingers around 100,000 cases.
"To our knowledge our estimate is the first ever scientific estimate of the national incidence of this infection in Egypt. We welcome the publication and dissemination of any other scientific estimate with a clearly stipulated methodology," said Abu-Raddad.
"Even if [new cases per year] were 100,000 – the issue is why should there be such a huge number of incident cases for an infection that is relatively easy to prevent?" he added.
Rather than focusing on the public, we should direct these awareness campaigns to the doctors and dentists
Bilharzia, a disease caused by a parasitic Schistosome worm, is endemic to Egypt since the time of the Pharaohs. The HCV epidemic in Egypt is widely believed to be an unintentional consequence of a World Health Organization programme to treat Bilharzia patients in rural Egypt between the late 1950's and early 1980's. Reuse of non-disposable glass syringes with poor sterilization practice may have spread the virus, which is transmitted through blood-to-blood contact.
"The Bilharzia treatment programmes were only an indicator. But what was going on was thousands of injections for many other reasons with the same lax precautions, such as vaccines or testing for diabetes," explained DeWolfe Miller, an epidemiologist at the, University of Hawaii, and lead author of the study.
Several decades after the Bilharzia treatment programmes were discontinued, the virus continues to spread, making Egypt the country with the highest prevalence worldwide.
"It is ironic because Egypt has had medical universities and a huge professional healthcare system incomparable to other similar countries. This was a blessing, but that came with a price," said Miller.
Most people agree that the spread of the virus corresponds with the expansion of "modern medical care," he explained. "After all, no one knew about a blood borne virus called HCV. In Egypt, they had big campaigns for injections such as for Bilharzia, a large healthcare system and a large population. The virus got into the blood supply."
"I think a fundamental reason [for the high incidence of the virus] is the high prevalence of the infection to begin with – or the infection reservoir," added Abu-Raddad. "The contribution of the past practises, most notably the anti-Bilharzia programmes, has fueled a large prevalence. In Egypt, one out of every 10 people is infected and a carrier of the virus. So the chance of transmission is much higher [than in other countries]."
While working with an Egyptian team in 1992, Miller found that 10 % of first-time blood donors tested positive for Hepatitis C. Miller then spent many years in Egypt, visiting healthcare facilities all over the country to study the virus as an epidemiologist.
"But I became more interested in working in intervention in Egypt, and that is what drove me to do this. I really want to have an opportunity to participate in a project in Egypt on prevention. This would be the greatest thing I can ever do right now."
There are regular HCV awareness campaigns in Egypt explaining modes of infection and how to protect against infection. However, the PNAS report suggests that the virus continues to spread in Egypt mainly through iatrogenic transmission.
"The public awareness programmes are not actually directed at the right people. They are directed at the public, and the public are not the ones causing the transmission. This is a blood-borne virus, and ordinary laypersons are usually not sharing their blood," explained Miller.
"Rather than focusing on the public, we should direct these awareness campaigns to the doctors and dentists," said Ramy El-Samman, a dentist who runs a private clinic in Cairo, Egypt. "We need to focus on who is behind the infection, not the patients."
The Ministry of Health and Population (MOHP) started an HCV prevention programme a few years ago which has been fairly successful. But Miller thinks there is more that can be done.
"It is a large health system and not all of it is being covered. Egypt is dedicated to a big treatment program, but they still need to invest more resources and energy into prevention at the level of healthcare delivery," he added.
According to El-Samman, prevention is now an important topic in medicine and dentistry education. Thus the younger generation in the healthcare sector follows more stringent standards. Older, more well-known doctors, however, do not follow these standards as well.
"I expect that quality control may not be rigorous enough. At the end of the day it comes down to the doctor himself," added El-Samman.
MOHP has a large budget for its HCV treatment programme. Miller suggests that diverting some of these resources to prevention would pay off big time.
"We already have many models for this. It is neither something completely new nor something we need to invent."
The preferred treatment regimen for Hepatitis C is a 48-week course of interferon and the antiviral drug ribavirin. The course costs around 3,500 USD, well above what the average family in Egypt can afford. It is usually only effective in 30-50% of cases. Many people receive subsidized treatment with a heavy burden on the healthcare system.
Miller has been trying to get funding for a project to make prevention a cornerstone of the response to the epidemic in the healthcare and dental care systems. His proposed project would provide information on Hepatitis C to the national education system to inform the general population on what precautions their doctors and dentists should be taking to prevent infectious diseases.
"The patients now have enough awareness [of Hepatitis C] to ask their dentists about prevention methods, but maybe it is not widespread enough," said El-Samman. "However, in the public sector, doctors can be very offended to have their patients ask them such questions."
In addition to the public, Miller wants to educate healthcare workers on how to minimize infection through his project. He wants to raise money from the US to counter what he sees as the most serious healthcare challenge facing Egypt.
"I'm at a point where I don't want to be publishing research anymore, I want to be doing something about it."
doi:10.1038/nmiddleeast.2010.188
Stay connected: